At some point or another, most women have experienced some form of urinary incontinence.
Sometimes, it’s a complete lack of control that results in the person wearing absorbent pads or discreet adult diapers. Other times, it’s bladder leakage or “little dribbles,” as some of our customers have described them to us.
Regardless of the amount of liquid they’re dealing with, it can feel embarrassing. It doesn’t matter how normal or common bladder leaks are, women are still embarrassed by it.
In fact, they’re often so embarrassed that they don’t even tell their doctors. They choose to live with it instead.
There are many different reasons why women suffer from urinary incontinence. Some are preventable — and also treatable — while others are less so.
The most important thing to keep in mind is that you’re not alone and that there may be something you can do to improve your quality of life.
Let’s talk about why urinary incontinence occurs, why it tends to happen when you cough (or laugh, or sneeze), and what you can to do treat it.
Why Do I Pee When I Cough? (Or Laugh… Or Sneeze)
While there could be many reasons you may be peeing when you cough, laugh or sneeze, it probably has to do with your pelvic floor.
If you experience bladder leakage while coughing, laughing, sneezing, or exercising, it’s medically classified as stress urinary incontinence.
During all of these activities, your pelvic floor engages. You may be able to feel these muscles tighten and then release (assuming you know which muscles to be cognizant of).
Because your pelvic floor muscles are there to support your bladder, bowels, and uterus, sudden contraction or relaxation of these muscles can trigger your bladder to leak.
3 Common Causes of Urinary Incontinence in Women
Assuming there is no other physical trauma or underlying medical condition at play, there are three major causes of urinary incontinence in women: pregnancy, childbirth, and menopause.
Pregnancy
It’s common for women to assume that childbirth inflicts the most trauma on their pelvic floor — and with good reason. While childbirth can certainly strain your pelvic floor, pregnancy can be just as hard on this critical set of muscles for multiple reasons.
During the standard 40-week pregnancy, your body is becoming more and more accustomed to the growing fetus inside of it.
Your organs are slowly moving out of the way to make room. Your hormones are preparing your body for childbirth and parenthood. You’re gaining weight — not because of cravings or late-night snacks (although, maybe some of that, too) — but because the fetus is getting bigger, the placenta has been developed, and your blood supply is increasing.
All of this activity is extra. Your body doesn’t do this on a normal basis, and therefore, your pelvic floor muscles aren’t used to carrying the extra weight. 
Because the fetus grows rather slowly, there’s a chance for our pelvic floors to adjust accordingly. However, the last 4-8 weeks of pregnancy are often the most difficult, in large part because your body is running out of room.
It’s during these final weeks of pregnancy that the fetus’ main job is to grow. A significant portion of the development has already occurred and everyone is just waiting for the fetus to gain weight and announce their intent to vacate their cozy home.
Furthermore, all those pregnancy hormones are doing a number on your body so they can prepare the body for your child’s impending arrival. It’s these hormones that eventually help you produce breastmilk, help your body heal, and give you that mama bear instinct.
What do Pregnancy Hormones Have to Do with My Pelvic Floor?
Another function of these hormones is to soften your pelvic floor to make childbirth easier (not that it’s ever “easy”). Loosening the muscles should help facilitate the actual pushing — after all, pliable material is easier to stretch than a rigid one.
That’s all well and good, but in the meantime, this extra elasticity isn’t doing your bladder any favors.
Without its regular support, your body may not be able to realize that your bladder is full. Either you won’t be able to tell, or your bladder is so restricted by your ever-growing uterus that it can’t get very full and the need to urinate happens frequently and urgently.
Of course, you’re also drinking more water than ever before in your life, which will make you urinate more frequently.
There aren’t many other points during a woman’s life when will there be a 7-10 pound weight constantly putting pressure on their bladder and pelvic floor. (Not to mention, a fetus using nearby organs as soccer balls like a World Cup champion.)
With all that added strain and extra hormones loosening things up, it’s no wonder that some pregnant women experience incontinence. This could be stress or urge incontinence, or a combination of both.
Childbirth
Childbirth is one of the more physically traumatic experiences a woman can go through. You’re pushing a 7-10 pound baby out of your body. It’s difficult. There’s no way around it.
Unless you have a scheduled cesarian section or you’re rushed into an emergency c-section, you’re going to have your baby traditionally.
While women often worry about the effect childbirth will have on their bodies, it’s the pelvic floor that ends up taking the brunt of the force.
Because your pelvic floor will already be strained from carrying the added weight of a fetus and your pregnancy hormones will have relaxed the muscles, the act of pushing the child out can further damage the muscles.
The other complication is the length of your labor, specifically the second stage, which is the pushing portion of the experience. Beforehand (in the first stage) your cervix is dilating and afterward (stage three), you’re delivering the placenta. And let’s be honest, that’s nothing after a whole baby. Stage three won’t have much of an impact on your pelvic floor.
Menopause
Much like during pregnancy, menopause is a time in a woman’s life when hormones are raging. Unlike pregnancy, hormone changes during menopause are meant to slow the body down.
Hormonal changes during menopause will cause muscles to weaken, including those in your pelvic floor.
Furthermore, body tissue (including the tissue that makes up your organs) weakens and loosens with age. Between a weakened pelvic floor and a bladder losing its elasticity, the chances of urinary incontinence become more likely than not.
Other Possible Causes of Urinary Incontinence in Women
There are plenty of reasons women could experience urinary incontinence. If they aren’t the three we’ve already discussed, the cause is likely one of the following.
Physical Strain or Injury (Other than Childbirth)
The pelvic floor is a series of muscles surrounded by tendons and nerves, so any kind of trauma to these components could cause urinary incontinence — “anything that affects the nerves and muscles of the pelvic area,” says Dr. Brynna Connor, Healthcare Ambassador at NorthWestPharmacy.com.
Obviously, childbirth can be included as a physical strain or injury, but for the purposes of this discussion, Dr. Connor is referring to other circumstances. Accidents that cause physical injury (car, bicycle, etc) could damage the pelvic floor, as could surgery.
To that end, we could include cesarian sections in this category. While women may not have gone through traditional childbirth or had to push at all, c-sections come with a risk of injury to the pelvic floor.
Medical Conditions
There are a few medical conditions that can cause urinary incontinence in women. One rather common one is some sort of obstruction, such as a urinary stone (like a kidney stone, but in your bladder) or tumors along the urinary tract. Obstructions like these can cause little leaks.
Neurological disorders can also be a cause of urinary incontinence. Conditions such as multiple sclerosis, Parkinson’s disease, or brain tumors can cause bladder leakage and/or lack of bladder control entirely.
Other possible medical conditions that can cause incontinence include those that form as a result of damage to the brain or spinal cord.
This list is by no means comprehensive, as there are medical conditions that can exacerbate existing urinary incontinence (such as diabetes). Because people are more likely to have chronic conditions as they age, maintaining a strong pelvic floor is one way to help prevent urinary incontinence.
Medication
Alpha-blockers (often used to treat hypertension) can sometimes lead to urinary incontinence. The reasoning behind this side effect is two-fold: alpha-blockers dilate blood vessels and — specifically in women — they can relax the bladder.
Some antidepressants are helpful for women who experience urinary incontinence, others prevent full constriction of the bladder. Sometimes, this means that the bladder cannot completely empty, leaving urine behind and causing leaks when it fills up again. 
Diuretics are another class of drugs that can exacerbate urinary incontinence. Also known as “water pills,” the main purpose of diuretics is to flush the body, which leads to more frequent urination. Of course, this means any issues with leaks or dribbles are likely to get worse.
Sleeping pills can also contribute to bladder leakage because patients don’t necessarily feel the need to urinate while they’re sleeping. Typically this is only an issue overnight — not during waking hours.
How to Say Goodbye to Bladder Leakage for Good
Many women think that bladder leakage or urinary incontinence is just something they have to live with. It feels inevitable.
And then even if (not when) they begin to experience little dribbles, they’re often too embarrassed to bring it up with their physician.
Generally, the earlier you begin your pelvic floor training, the better. If you’re fortunate enough to know the role your pelvic floor plays in your overall and feminine health at an early age, starting pelvic floor exercises is a great idea.
You don’t have to wait until after you have children, nor is menopause too late to start strengthening your pelvic floor.
If you’re looking for a pelvic floor device to assist with Kegel exercises, look no further than the Yarlap device with Autokegel technology.
Award-Winning Yarlap Device with Autokegel Technology
The reason we often point out that people don’t always know which muscles to pay attention to during Kegel exercises (or when they cough, laugh, sneeze, or exercise) is that, well… it can be difficult to tell. And it’s not as if someone can show you the same way they’d demonstrate how to perform a proper deadlift. 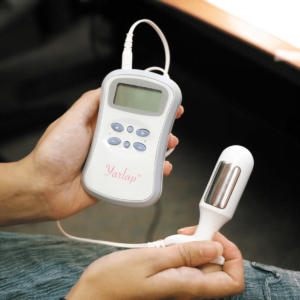
Women have a hard enough time gathering the courage to talk about incontinence with their physicians. If the response they get is “just do Kegel exercises” and they don’t even know how to do them, how likely do you think they’ll be to ask additional questions?
This type of response may seem simple to a physician who has all the knowledge they do about human anatomy. But if you’ve never done Kegel exercises and you’re not attuned to the intricacies of your pelvic floor, you may literally not know how to do Kegels.
As a patient, you may feel as though your concerns have been dismissed. And these feelings may prevent you from continuing the discussion, or even asking your close friends.
It’s exactly for this reason that we developed the Yarlap device with Autokegel technology. You don’t have to know how to properly do Kegels — the Yarlap device will do Kegels for you, perfectly, every single time.
Important Considerations Before Trying the Yarlap Device
While the Yarlap device has already been helpful for millions of women, there are circumstances under which it may not be right for you.
First and foremost, the Yarlap device should not be used if you have a pacemaker.
Second, if you’re pregnant, be sure to consult with your OB/GYN before using the Yarlap device. Physicians tend to err on the side of caution when it comes to pregnancy (with entirely good reason), and they’re likely to recommend you wait to try Yarlap until after your 6-week postpartum visit.
Are You Ready to Yarlap?
If you’re ready to banish urinary incontinence or little leaks forever, the Yarlap device may be able to help you.
Yarlap is private and completely discreet.
You won’t need to use an app (with the potential to be hacked), as the entire device is self-contained.
You also won’t need to be concerned that people will notice what you’re doing. We have one customer who watches the news with her husband every single night. During that time period, she Yarlaps — and he has no idea.
If you’d like to learn more about our award-winning Yarlap Autokegel device, we’re more than happy to help you. We’re happy to answer any questions over the phone, or you can check out our frequently asked questions page.
But if you’re ready to purchase, you can do so on our website, or just give us a call at (614) 568-7000. We’re looking forward to helping you!
DISCLAIMER: THIS WEBSITE, YARLAP, AND RLI, INC. DO NOT PROVIDE MEDICAL ADVICE OR DIAGNOSIS.
The information, including but not limited to, text, graphics, images and other material contained on this website are for informational purposes only. Any information published on this website or by this brand is not intended as a substitute for professional medical guidance and should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. Always seek the advice of your physician or other qualified health care provider with any questions you may have regarding a medical condition or treatment and before undertaking a new health care regimen, and never disregard professional medical advice or delay in seeking it because of something you have read on this website. Links to other sites are provided for information only – they do not constitute endorsements of those other sites or any recommendations or advice contained therein.


